Those with advanced disease or SS often require multiple lines and recurrent courses of systemic therapies. Patients with early-stage disease typically receive skin-directed therapies, such as topical steroids, UVB and PUVA phototherapy, and local radiation. She added that management often requires a multidisciplinary team of specialists in dermatology, hematology/oncology, dermatopathology, and radiation oncology who have expertise in cutaneous lymphoma, especially for those with advanced disease. It can take many years to confirm a diagnosis of cutaneous T-cell lymphoma.” 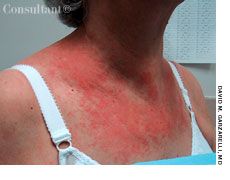
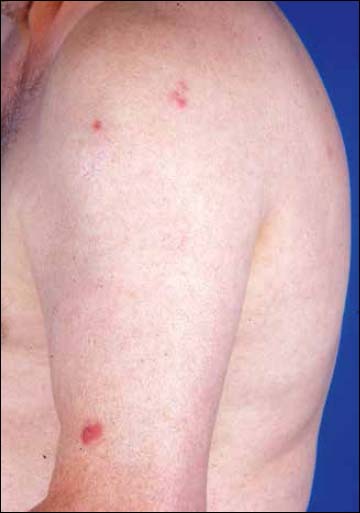
“Sometimes 1 biopsy is not enough,” Chen said. At this point, CTCL can look like several skin conditions, making it one of the most challenging diseases to diagnose. Pei-Ling Chen, MD, PhD, a member of the Pathology and Cutaneous Oncology Departments at Moffitt Cancer Center and a member of the Moffitt Cutaneous Lymphoma Multidisciplinary Clinic, recently published a new study done in patients with CTCL with large cell transformation (transformed CTCL) this occurs when a specific subset of MF tumor cells undergoes molecular and/or genetic changes that cause them to become an aggressive large cell lymphoma.Įarly-stage disease presents with scaly patches alone, or patches and plaques of different shapes and sizes, commonly located on the sun-protected areas of the body. These trends hold even after accounting for disease characteristics, socioeconomic factors and treatments received. 
8 Large-scale SEER and National Cancer Database studies showed that Black/African American patients have a higher incidence rate, younger age of onset, higher disease burden, and inferior survival compared with their White counterparts. Men are more likely to develop the disease compared with women (overall annual age-adjusted incidence, 8.7 × 10 -6 vs 4.6 × 10 -6). Median age at diagnosis is 55 years to 60 years, and risk increases with age. Similar to Richter transformation in chronic lymphocytic leukemia, transformation in CTCL portends an immediate transition to aggressive clinical behavior-especially for those who transform within 2 years of MF diagnosis it is also linked with a rapid decline in survival and resistance to multiple forms of therapy. The primary site of detectable transformation is the skin. The incidence of LCT in patients with early-stage disease is 1.4%, compared with 27% in those with stage IIB disease and 56% to 67% in those with stage IV disease. Large cell transformation (LCT) occurs in a subset of patients with MF and Sezary syndrome, when the lymphoma cells undergo histopathologic transition from neoplastic small-medium sized lymphocytes to large, blast-like T-cells. Sézary syndrome, the leukemic variant of CTCL with circulating malignant T-cells in the peripheral blood, accounts for approximately 3% to 5% of CTCLs. 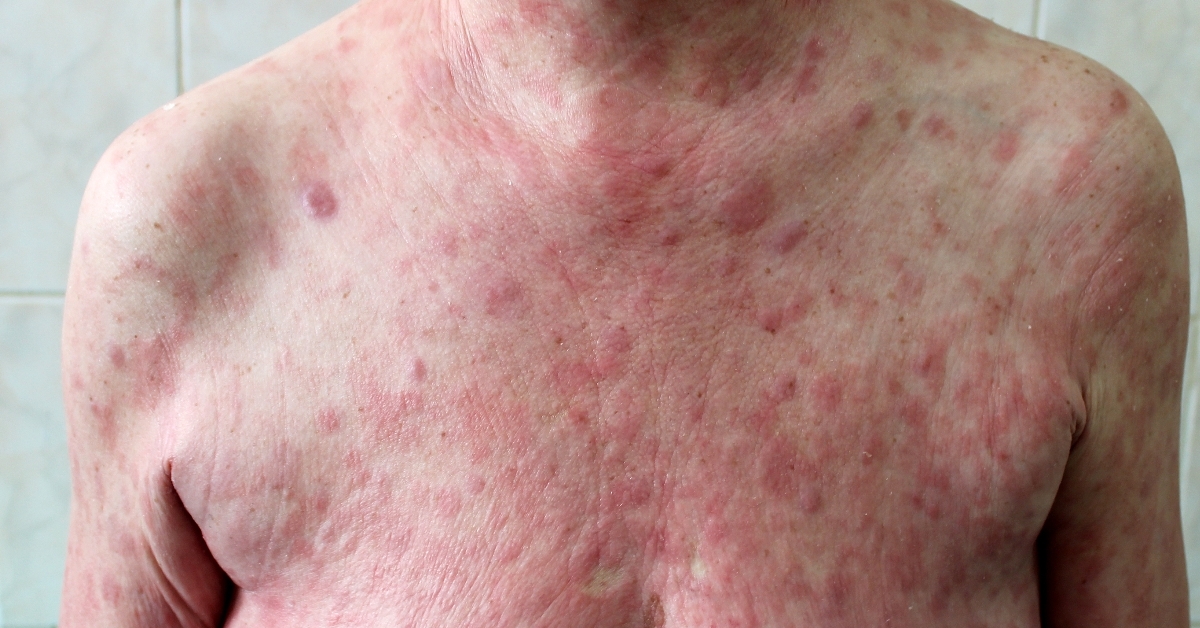
MF is characterized by cutaneous patch, plaque, or tumor lesions. The most common form of CTCL, mycosis fungoides (MF) accounts for upward of 60% of CTCLs. 1Īs reported by the Surveillance, Epidemiology and End Results (SEER) registry data, annual overall incidence in the United States was 6.4 cases per million persons from 1973 to 2002, increasing to 7.7 per million persons in 2001 to 2005. Over that same period, investigators also observed a trend toward increasing 5-year overall survival (OS) since 1973, plateauing at 78.3% from 1997 to 2005. Although cutaneous T-cell lymphoma (CTCL), a group of non-Hodgkin T-cell lymphomas, remains a rare disease, incidence has increased steadily since the 1970s.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
